Government Data Proves Raw Milk Safe
June 22, 2011Whole Life Buying Club, Kentucky
September 20, 2011By Ted Beals, MD
Remarks delivered at the Third International Raw Milk Symposium, May 7, 2011, Bloomington, Minnesota. See also Dr. Beals’ PowerPoint Presentation from this event (PDF).
I wish to begin by saying that the real discussion of food, including raw milk, should focus on the undeniable values and benefits for our development and sustained health. Sally Fallon Morell has talked about those in her presentation, and my role here is to focus on the risk aspects, which are controversial.
Most of us here are convinced that what we eat, and why we choose to eat what we eat is our responsibility, not the responsibility of government. Yet the government is at war against raw milk, one of the key healthy foods that we choose to consume and give to our children.
The government’s battlefield is the concept of risk—raw milk is inherently risky, argue government officials, and should not be consumed by anyone, at any time, for any reason. Some of our opponents in this battle understand the importance of nutrition and realize the incredible power held by those that control food. Others go to work every day sincerely believing that they are personally responsible for protecting the public from the risks associate with eating. Many regulators, inspectors, lawyers and far too many legislators tend to forget about the benefits and focus on the things that might make people sick, and they call those things “bad bugs.”
But everything has risk. The decision to consume any food involves estimating the risks of eating that food, as well as the benefits. Eating is not just an interesting thing we do, like riding in airplanes; rather, it is an absolute necessity. And many of us believe that our well being is a direct consequence of the food choices we make.
Today I will present the actual scientific facts stripped of the hysteria and devoid of unsubstantiated dogma. I will do so in a way that all of you will understand; what I am presenting is not my opinion; it is the actual scientific information.
Bacteria Are Ubiquitous
The world is filled with bacteria. They are on our skin and in our digestive system. They are everywhere. Bacteria are absolutely essential to our development, our ongoing nutrition and our health. Bacteria are not determined to make us sick, they are just looking for a place to grow and divide. Here are some key facts about bacteria:
- Bacteria outnumber people.
- They were here long before us.
- They will be here long after us.
- They dominate the diverse bio-culture of the world.
- Our existence is integrated with that of bacteria.
All the bacteria in our world today have succeeded over a long period of history to find nice places to grow and divide. When we came along, a small number of them found that humans have some nice places wherein to grow and divide.
The bacteria that live inside and on human beings either just co-exist with us, or we have actually learned to use their presence to our advantage.
A surprisingly small number of those bacteria may cause side effects (collateral damage) when they grow and multiply.
In the whole world, there are hundreds of thousands of different kinds of bacteria, and a million trillion trillion individual bacteria. Of those bacteria that live on and inside human beings, there are hundreds of different kinds. In fact, there are more bacteria on and in our bodies than we have cells of our own.
The vast majority of these bacteria—hundreds of kinds—are beneficial. And how many kinds of bacteria might make people sick? The answer is surprising: only a couple of dozen. And only some of these actually cause illness.
The official naming system for bacteria gives the genus and species. For example with Listeria monocytogenes, Listeria is the genus and monocytogenes is the species. However there is abundant diversity within these officially named categories in the form of subtypes. There are different categories of subtypes: serotypes, genotypes, strains, forms, serovars, virotypes, varieties and isolates. For example, the highly publicized form of Escherichia coli (remember nearly all forms are benign) is Escherichia coli O157:H7. This expanded name says: the genus is Escherichia, the species is coli, and within the category of O subtypes of the species coli it is number 157, and within the category of H subtypes it is number 7.
All bacteria named with genus and species have subtypes!
The Myth of the Risk Mongers
A critical myth perpetuated by the risk mongers is that all of the subtypes in a named (genus and species) of bacteria are the same. This is how the myth works. If there is disease in some animal or man and the laboratory identifies the cause as a certain genus and species, then that makes it a “pathogen” and any and all bacteria of that genus and species cause disease. They want judges, legislators, journalists and the public to believe that the genus and species is a bad bug and must be killed. Thus, goes their logic, since one subtype of E. coli can make people very sick, then all subtypes of E. coli are pathogens and cannot be tolerated.
Yet, thousands of researchers, hundreds of books and thousands of published articles in scientific journals, all recognize the scientific fact that just because a particular subtype of a bacteria species is pathogenic does not mean that the whole species is pathogenic.
The risk mongers understand that their horror stories crumble in the face of truth, scientific facts and reality. So they keep repeating this myth to journalists, legislators and judges. Every time they say anything about possible illness, they repeat this myth. Some even imply that all bacteria are bad.
The Big Four
Let’s now take a brief look at each of the four dreaded “pathogens” that cause most foodborne illness—Campylobacter jejuni, Shiga Toxin producing E. coli (E. coli O157:H7), Listeria monocytogenes and Salmonella spp. (spp. Indicates that we are talking about the whole genus of Salmonella, not just one species.)
For each one, we need to know the following:
- Where do they like to grow?
- What is the most common source?
- What is the most common reservoir?
- Factors that increase potential risk to raw milk drinkers;
- Factors that decrease potential risk to raw milk drinkers;
- Overall human public health impact from each pathogen;
- The specific public health impact from each pathogen associated with drinking milk raw.
Campylobacter Jejuni
The most common pathogen currently associated with raw milk outbreaks is Campylobacter jejuni. The virulent forms of Campylobacter jejuni can cause serious diarrhea in humans.
Campylobacter jejuni grows only inside living animal cells. The most common source is the intestinal tract of poultry. Infected chickens are not sick, but they are carriers of the organism in their feces and on meat contaminated with feces. The most common reservoir is water contaminated from poultry manure. People with diarrhea caused by Campylobacter jejuni shed extremely high concentrations of the virulent bacteria in their stools.
Ironically, the potential risk is increased with raw milk that is too fresh. Over time, the antimicrobial components of raw milk will kill Campylobacter jejuni, so—any potential risk diminishes as the milk ages under refrigeration. Longer storage time and exposure of the milk to air decrease the risk to raw milk drinkers. Likewise keeping infected poultry and people that carry campylobacter away from milk handling areas will reduce the risk.
Campylobacter is the second most common cause of all human foodborne illness. The illness usually goes away without treatment after a bout of unpleasant diarrhea, but there can be severe complications in rare cases.
As for the specific public health impact of drinking raw milk, the Centers of Disease Control (CDC) estimates an annual average of more than eight hundred thousand (845,024) people in the U.S. have domestically acquired diarrhea caused by food contaminated with Campylobacter spp.1 an annual average of 34 Campylobacter jejuni illnesses have been attributed to drinking raw milk.2
Shiga Toxin-Producing E. Coli (E. Coli O157:H7)
This pathogen grows in the intestinal tract of warm blooded animals. The most common source is fecal matter of infected humans. The most common reservoir is cows that are shedding colonized virulent subtypes.
Factors that increase the risk to raw milk drinkers include dairy animals contaminated with feces from high-shedding animals and milk handlers shedding during and after infection.
Factors that decrease the risk to humans include closed herds, managing dairy herds to minimize the spread of bacteria spread from colonized animals, and keeping people that are shedding away from milk processing and herds.
The overall human public health impact of E coli O157:H7 is small but highly publicized because of a rare side effect called hemolytic uremic syndrome (HUS).
As for the specific public health impact of drinking raw milk, CDC estimates an annual average of more than sixty-three thousand (63,153) people in the U.S. had domestically acquired diarrhea caused by food contaminated with E.coli O157:H7:1 an annual average of five were attributed to drinking raw milk.2
Listeria Monocytogenes
Listeria monocytogenes (often abbreviated to L. mono.) is the most serious and deadly of the contemporary foodborne pathogens. Yet it is also ubiquitous in our environment. Scientists actually know a lot about the virulence factors that are necessary before specific virulent subtypes of Listeria monocytogenes are able to cause disease.
Listeria monocytogenes can alternate between two growing modes: it grows within animal cells or it can switch to growing in decomposing plant materials. Listeriosis is a significant health problem in domestic animals. The most common sources are poorly managed silage; amniotic fluid, placenta and fetal tissues from abortions resulting from infection in cows; and meat processing plants and their equipment.
The most common reservoir is the environment, particularly if cool, wet and undisturbed. Listeria monocytogenes is present as well in our homes and on our bodies.
The public ingests listeria on a regular basis without becoming ill. You must ingest huge numbers of a virulent strain of Listeria monocytogenes to cause gastroenteritis.
Those who wish to ban all milk that is not pasteurized use the horrors (human listeriosis) of systemic disease caused by Listeria monocytogenes to support their cause. They consistently broadcast the high mortality rates from L. mono and focus on the susceptibility of pregnant women, fetuses, newborns and the elderly. However, Listeria monocytogenes has never been a significant public health risk from drinking fresh raw milk. Because of the long processing times and storage conditions, there have been rare outbreaks in which cheeses have been associated with listeriosis cases. This is a risk with cheeses prepared from both raw and pasteurized milk.
The most serious public health risk due to Listeria monocytogenes, comes from contaminated ready-to eat processed foods, particularly meats.
CDC estimates an annual average of fifteen hundred (1,591) people in the U.S. develop systemic infection caused by food contaminated with Listeria monocytogenes;1 there have been no cases attributed to drinking raw milk in the last twelve years.2
Salmonella Spp
Our final pathogen is Salmonella spp. It likes to grow inside animal cells as well as in food and feed with high protein content, especially when stored warm.
The most common source is infected humans and animals, as well as contaminated animal feeds and re-warmed foods. The most common reservoir is contaminated water.
Inadequate refrigeration of raw milk increases the risk to consumers; eliminating sources of salmonella decreases the risk.
As for the overall human public health impact, salmonella is the most common foodborne illness. CDC estimates an average of more than one million (1,027,561) people in the U.S. had domestically acquired diarrhea caused by food contaminated with salmonella1—an annual average of three of these cases were attributed to drinking raw milk.2
Relative Risk of Drinking Raw Milk
First a personal note. I have performed the calculations based on national highway safety data and the data on foodborne illness attributed to drinking raw milk. It can be shown that I have a greater risk of being injured in the car driving to the farm to obtain milk for myself and my wife than becoming ill from the fresh unprocessed whole milk. And we drink a lot of that delicious and healthy milk every day.
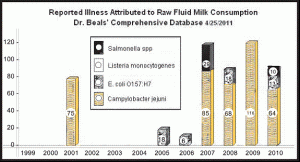
Now, let’s look at the risk of consuming raw milk compared to other foods. I have combed all available information including scholarly articles, reviews of foodborne illnesses, media reports, public health announcements, listings of outbreaks compiled by numerous government agencies, special interest groups and litigation lawyers and found the following data on total annual illnesses attributed to raw milk from 1999 through March 2011, a period of twelve years, as shown in Figure 1.2
Figure 1
For the period, there were 502 cases of illness, for an average of 42 per year. It is important to note that these illnesses were attributed to raw milk in the opinion of the reporting agencies. I have not excluded any illnesses from these numbers based on my professional judgment of the strength of the linkage reported. They include totals, both “confirmed” and “presumed” cases.
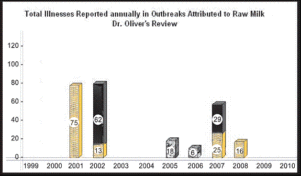
For comparison for those who insist on published data in peer reviewed journals, another set of data was compiled by Stephen P. Oliver and others entitled “Food Safety Hazards Associated with Consumption of Raw milk, published in Foodborne Pathogens and Disease.3 Oliver looked at illnesses attributed to raw milk over a nine-year period, 2000 to 2008, as shown in Figure 2. The numbers listed are those attributed to drinking fluid milk, and do not include illnesses attributed to other processed dairy products.
Figure 2
Ironically, Oliver and his team come up with a lower total than I did—246 cases over nine years, for an average of 27 cases per year. As you can see, there is no pattern for the frequency of illness attributed to drinking raw milk in either Figure 1 or Figure 2. With the exception of the more likely occurrence of Campylobacter jejuni illness and the absence of illness from listeria, the presumed causative organism and the frequency of illness is sporadic.
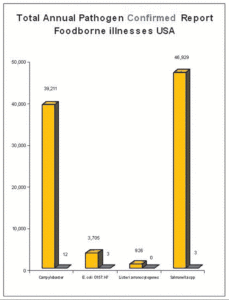
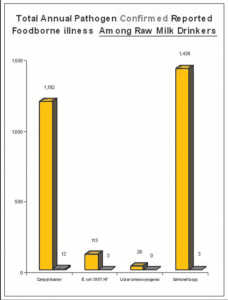
Figure 3 shows the annual incidence of foodborne illness confirmed for each of the four pathogens. Figure 4 shows illnesses confirmed for each of the four pathogens attributed to foodborne illness that might be expected among raw milk drinkers.
Figure 3
Figure 4
The numbers for illness from all food sources is data from a U.S. government report called Healthy People 2020.4 The report was finalized in December 2010 out of a collaboration of all health and food agencies of the federal government, with private sector input. In the section on food safety of this report, data is given for “baseline” 2010. The baseline in the report is given as a rate per one hundred thousand people in the U.S. In the graphs, the tall bars are totals attributed to “all foods” based on these rates using 2010 census population data. Critics of all data showing low numbers of people ill from drinking raw milk comment that since there are so few people drinking raw milk, the numbers only appear small. To counter this assumption, the numbers used in Figure 4 are also calculated using the 2010 Census and the Healthy People 2020 baseline risk of illness from all foods.
To construct Figure 4, we need to know the number of raw milk drinkers in the U.S. Fortunately, this data is available to us, and the number is surprisingly large. According to a very large telephone survey by FoodNet, carried out in 2007, 3.04 percent of the population consumes raw milk or about 9.4 million people based on 2010 census.5 This number is certainly larger today as raw milk is gaining in popularity; however, we can be conservative and use the percentage in 2007 from the phone survey of 9.4 million Americans consuming unpasteurized (raw) milk for the year 2010.
While it is true that only a minority drink raw milk, Figure 4 still shows the striking comparison between illness from all foods, and the incredibly small numbers attributed to drinking raw milk. In this graph I made the assumption that the risk of illness from all food sources was the same for people drinking raw milk. I personally suspect that raw milk drinkers as a whole are healthier and more immune than the general public, but the Healthy People 2020 did not actually make a calculation for the subset of the population that drinks raw milk.
As you can see, the number of illnesses from raw milk is very low compared to illnesses from other causes, both for all consumers and for raw milk consumers.
Illnesses Per Person
Now, let’s look at the illnesses per person among the whole population and the population of raw milk drinkers. That data showing illnesses come from a 2011 publication compiled by a team of researchers at the CDC FoodNet Surveillance Center. The paper, by Elaine Scallan and others, is entitled “Foodborne Illness Acquired in the United States—Major Pathogens” and was published in Emerging Infectious Diseases.6 The model does include a factor for unreported illnesses, but it revised downward the figure of 78 million foodborne illnesses per year that government agencies have been using in the past. Instead the report estimates that 48 million Americans are sickened each year from all agents, including viruses, bacteria and toxins, in all foods. That is one out of every six people. The numbers given in the report are based on their most up-to-date information which was for the year 2008. Their data:
| Total diarrheal episodes annually USA | 217,973,045 |
| Total foodborne illnesses annually USA | 48,000,000 |
| Annual confirmed foodborne infections from the four “pathogens” (all foods) | 1,937,561 |
| Average number of illnesses attributed to consuming raw milk (Dr. Beals, 1999–2011)2 | 42 |
| Average number of illnesses attributed to consuming raw milk (Drs. Oliver and others, 2000–2008)3 | 27 |
Who’s Irresponsible?
From the perspective of a national public health professional looking at an estimated total of 48 million foodborne illnesses each year;6 or from the perspective of a healthcare professional looking at a total of 90,771 (data from Healthy People 20204) confirmed bacterial foodborne infections each year (about 0.2 percent), there is no rational justification to focus national attention on raw milk, which may be associated with an average of 42 illnesses maximum among the more than nine million people (about 0.0005 percent) who have chosen to drink milk in its fresh unprocessed form.
Using this average of 42 illnesses per year, we can show, using government figures, that you are about 35,000 times more likely to become ill from other foods than you are from raw milk.
Calculations on Relative Amounts of Illness from Foods for Persons Drinking Raw Milk
It is irresponsible for a senior national government administrator to testify that because of those forty-two people, raw milk is inherently hazardous, parents should not be allowed to decide which foods they serve their children and milk should be banned across the nation unless it has been pasteurized.
SIDEBARS
Source Versus Reservoir
Another of the critical myths perpetuated by those who promote fear is that bacteria grow remarkably fast. The most common example used is the statement that E. coli multiplies every 20 minutes; suggesting that this is how all bacteria behave. The implication is that even if there is only a single bacterium, it will rapidly multiply producing alarmingly high numbers to spread infection. Yes, in a laboratory you can get E. coli to multiply that quickly if you put it in its most favorable environment, with abundance of all the desired nutrients, at the optimal temperature for growth (99 degrees F) and the right mixtures of gases. But just for comparison, Listeria monocytogenes divides once every fifteen to thirty-four hours at refrigerator temperatures in packaged meat slices. For the purposes of this discussion, bacteria can multiply, or if conditions are not favorable, they will diminish in numbers. So experiments either show increasing or decreasing numbers over time. In publications they may say “growing” to mean multiplying, and “surviving” to mean diminishing in numbers.
And for the purposes of this discussion, a “source” is a location that has conditions under which the specific virulent bacteria significantly increase in numbers. A “reservoir” is a location in which a specific virulent bacteria is able to survive for some time or has conditions to enable very limited multiplication.
Gastrointestinal Illness
As a physician, I am dedicated to understanding, preventing and minimizing the impact of disease. Gastroenteritis has a real personal impact. Frequent trips to the bathroom, often with terrible abdominal pain, inability to go about your daily activities, lasting for days, is serious. The fortunately rare complications that can occur periodically with the forms of gastroenteritis mentioned here can be horrific and have a devastating impact on individuals and their families. In no way do I wish to trivialize the personal impact of these illnesses. However, all activities have risk. Consumption of any food has some risk of illness or adverse reaction. And the consequence of basing public policy on horrific personal experiences is that all foods will ultimately be banned, and we will not be able to participate in any activity.
REFERENCES
- Scallan E, Hoekstra RM, Angulo FJ, Tauxe RV, Widdowson M-A, Roy SL, et al. Foodborne illness acquired in the United States—major pathogens. Emerg Infect Dis. 2011 Jan. Table 2 cdc.gov/EID/content/17/1/pdfs/09-1101p1.pdf
- Average annual illnesses attributed to drinking raw milk are from a comprehensive database of outbreaks attributed to raw milk started in Jan. 1, 1999. This database includes all incidents that have been included in any publication or review concerning raw milk outbreaks, newspaper reports, press releases, attorney webpages, lists compiled by interested groups and state and federal agencies as well as presentations at conferences or on TV. The numbers listed here are obtained from this dynamic database as of March 25, 2011. Additional incidents and updated information are being added to this database on an ongoing fashion. In this discussion the annual averages for each “pathogen” include all illnesses (confirmed and presumptive) reported in summary or final reports that have been made public. The annual average numbers of illness include only cases that occurred in the USA and were attributed to drinking raw milk that was produced specifically for consumption by people in the fresh unprocessed form. The numbers do not include cases attributed to dairy products other than fluid whole milk. I did not make a personal judgment to determine if the cases were proven to be caused by virulent pathogens in the milk. Attribution used in calculating the annual averages is solely at the determination of the reporting agency that made the final report. It should be noted that since the database is ongoing; the numbers will change at future points in time because new incidents are added as they surface, and information is continuing to be added to incidents already included in the database.
- Stephen P. Oliver and others entitled “Food Safety Hazards Associated with Consumption of Raw milk, published in Foodborne Pathogens and Disease. Volume 6, Number 7, 2009.
- Healthy People 2020.
- Centers for Disease Control and Prevention (CDC). Foodborne Active Surveillance Network (FoodNet) Population Survey Atlas of Exposures. Atlanta, Georgia: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, 2006-2007. cdc.gov/foodnet/surveys/FoodNetExposureAtlas0607_508.pdf
- Scallan E, Hoekstra RM, Angulo FJ, Tauxe RV, Widdowson M-A, Roy SL, et al. Foodborne illness acquired in the United States—major pathogens. Emerg Infect Dis. 2011 Jan. Table 2 cdc.gov/EID/content/17/1/pdfs/09-1101p1.pdf


11 Comments
Hello,
Is there a good reference source for a full list of bacteria found in raw milk? I can’t find a good source which lists good bacteria…
Sally Fallon Morell replies: There are probably hundreds of types of bacteria in milk–most of them of the beneficial lactic-acid producing type.
Dr. Beals, why are you comparing *actual* (even suspected actual) cases of illness from raw milk (42 avg per year) with an *estimate* of 48 million foodborne illnesses per year? That is outrageous manipulation of statistics. You need to compare *actual*/suspected cases of illnesses from all sources with those from raw milk.
The foodborne illness data is from the CDC FoodNet Surveillance Center. All population level data like this are estimates, but the CDC figures are the best available. The raw milk figures are “actual” only in the sense that they were taken from reports of actual outbreaks from various sources, but the population level number is still an estimate. The two are, in fact, quite comparable. It is not a “manipulation” of statistics. Of course, if you know of a way to better collect “actual” food illness in 320,000,000 people, the CDC would love to know!
A population estimate has a multiplier of some sort on top of actual reported illnesses to account for underreporting. So you can’t compare the two stats without first figuring out how to get a comparable multiplier.
So is there any point to bacteria, standard plate count and coliform testing for a producer’s raw milk? Is it necessary, do you think?
Its good to read this article. I believe that there are a lot of hype and scare tactics in what is often posted on raw milk. I grew up drinking raw milk and feel so good when drinking it. Never had a problem.
Just the same, I think that if one isn’t clean with the production, one can cause bad bacteria to get into the milk.
What about lack of proper quick cooling of the milk?
From Sally Fallon Morell: Testing is important, to monitor the cleanliness of the milk and the dairy. The easiest is rapid testing for coliform, which can be done with every batch of milk. And yes, raw milk should be cooled down quickly.
This is a really great article that helps to quantify the risk of drinking raw milk. But, I think it’s only mildly helpful at best (silly, at worst) to compare raw milk sickness with sicknesses from spinach and chickens.
Isn’t the better comparison raw milk compared to pasteurized milk? Where is this study?
I don’t think it is a silly comparison; if it’s riskier to eat a number of common foods vs. raw milk, that’s relevant. If raw milk happened to be slightly riskier than pasteurized milk, but still far less risky than a number of common foods, that’s relevant. Sally will be hearing Ted Beals speak next month. He’ll be giving these comparative numbers and she is planning to report on them in a future WAPF journal article. Stay tuned.
Where is the comprehensive database mentioned in reference 2?
He is not sharing the database, but the bottom line is that there are about 42 reported (not proven) illnesses from raw milk per year.